How to Administer an Enema: Step-by-Step Nursing Procedure Guide
Meta Description
Learn how to administer an enema with this step-by-step nursing guide, including procedure, types, safety tips, and patient care best practices.

Enema administration is a fundamental nursing procedure used in hospitals, clinics, and home care settings. Whether for relieving constipation, preparing patients for diagnostic procedures, or administering medication, understanding how to safely and effectively give an enema is essential for every nurse.
This guide provides a clear, step-by-step approach to enema administration, along with important nursing considerations, patient safety tips, and best practices to ensure optimal outcomes.
What Is an Enema?
Relieve constipation
Cleanse the bowel before surgery or procedures
Administer medication
Reduce toxin buildup in certain conditions
Enemas work by stimulating bowel movements and softening stool, making it easier to pass.
Types of Enemas
Understanding the different types of enemas helps nurses choose the correct procedure based on patient needs.
1. Cleansing Enema
Used to remove feces from the colon.
Examples:
Normal saline enema
Tap water enema
Soap suds enema
2. Oil Retention Enema
Softens hardened stool and lubricates the rectum.
3. Medicated Enema
Delivers medication directly into the rectum (e.g., anti-inflammatory drugs).
4. Carminative Enema
Helps relieve gas and abdominal distention.
Indications for Enema Administration
Enemas are indicated in several clinical situations:
Severe constipation
Fecal impaction
Preoperative bowel preparation
Diagnostic procedures (e.g., colonoscopy)
Medication delivery
Relief of abdominal distension
Contraindications (When NOT to Give an Enema)
Nurses must carefully assess patients before administering an enema.
Avoid enemas in:
Recent colorectal surgery
Severe hemorrhoids
Rectal bleeding
Inflammatory bowel conditions
Suspected bowel obstruction
Always consult a physician if unsure.

Equipment Required
Before starting the procedure, gather all necessary supplies:
Enema solution (as prescribed)
Enema bag or pre-packaged enema kit
Lubricant (water-soluble)
Gloves
Bedpan or access to toilet
Waterproof sheet
Towels or wipes
Preparation ensures a smooth and efficient procedure
.Patient Preparation
Proper preparation improves patient comfort and cooperation.
Key Steps:
Explain the procedure clearly
Ensure privacy
Encourage the patient to empty bladder
Position the patient correctly
Place a waterproof sheet under the patient
Patient Positioning
The correct position is essential for effective enema administration.
Left lateral (Sims’) position is preferred because:
It follows the natural curve of the sigmoid colon
Promotes better flow of solution
Reduces discomfort

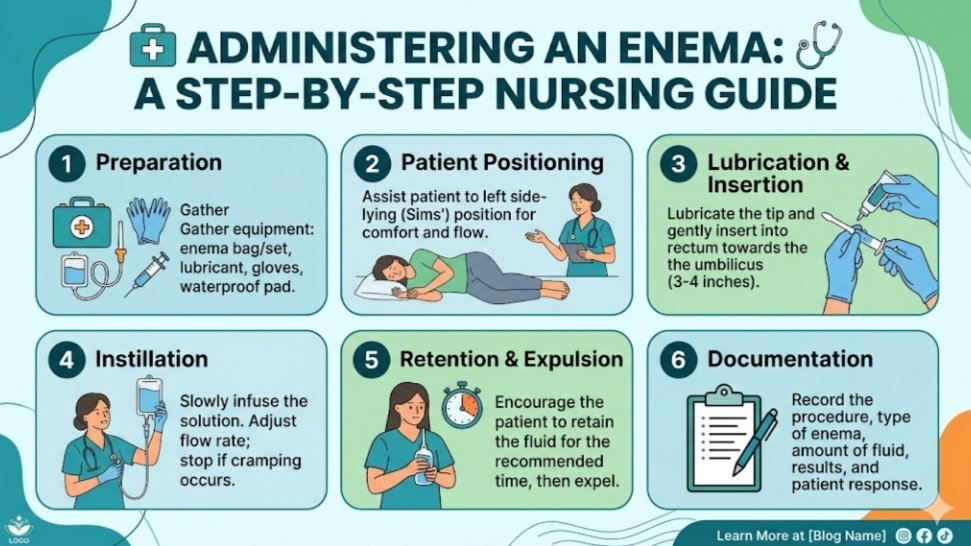
Step-by-Step Procedure for Enema Administration
Follow these steps carefully to ensure patient safety and effectiveness.
Step 1: Hand Hygiene
Wash hands thoroughly and wear gloves.
Step 2: Prepare the Solution
Warm the solution to body temperature
Fill the enema bag
Remove air from tubing
Step 3: Position the Patient
Assist patient into left lateral position
Flex the right knee
Step 4: Lubricate the Tip
Apply water-soluble lubricant to the enema tip.
Step 5: Insert the Tube
Gently insert 3–4 inches (7–10 cm) into rectum
Do not force insertion
Step 6: Administer the Solution
Raise enema bag about 12–18 inchesAllow solution to flow slowly
Monitor patient discomfort
Step 7: Clamp and Remove
Clamp tubing when solution is administered
Gently remove the tip
Step 8: Encourage Reten uution
Ask the patient to retain the fluid for 5–15 minutes if possible.
Step 9: Assist with Elimination
Provide bedpan or assist to toilet.
Step 10: Document the Procedure
Record:Type of enema
Amount of solution
Patient response
Outcome
Nursing Responsibilities During the Procedure
Nurses play a critical role in ensuring patient safety.Monitor for:
Pain or discomfort
Cramping
Dizziness
Signs of bowel perforation (rare but serious)Ensure:
Gentle technique
Proper communication
Patient dignity
Complications of Enema Administration
Although generally safe, complications can occur.Common Complications:
Abdominal cramping
Rectal irritation
Fluid imbalance
Serious Complications:
Bowel perforation
Infection
Electrolyte imbalance
Proper technique minimizes risks.

Tips for Safe and Effective Enema Administration
Always use correct solution type
Avoid excessive pressure
Maintain appropriate height of enema bag
Communicate with patient throughout
Stop immediately if severe pain occurs
Enema Administration in Special Populations
Pediatric Patients
Use smaller volume
Gentle insertion
Extra reassurance
Elderly Patients
Monitor for fluid imbalance
Use mild solutions
Bedridden Patients
Ensure proper positioning
Prevent skin breakdown

Importance of Communication in Nursing Care
Clear communication improves patient cooperation and reduces anxiety.
Explain:Purpose of the procedure
What the patient will feel
How long it will take
Empathy and reassurance are essential.
Accurate documentation is vital in nursing practice.
Include:Time and dateType of enema
Patient tolerance
Results
Any complications
Conclusion
Administering an enema is a fundamental nursing skill that requires knowledge, precision, and compassion.
By following proper procedures, maintaining patient dignity, and ensuring safety, nurses can effectively perform this procedure and improve patient comfort.
Whether in hospital settings or home care, mastering enema administration is an essential competency for delivering high-quality nursing care.
❓ Frequently Asked Questions (FAQs)
1. What is an enema and why is it used?
An enema is a procedure where fluid is introduced into the rectum to relieve constipation, cleanse the bowel, or administer medication. It is commonly used before surgeries or diagnostic procedures.
2. How do nurses safely administer an enema?
Nurses follow a step-by-step process that includes proper patient positioning (left lateral), using lubricated equipment, controlling fluid flow, and monitoring patient comfort throughout the procedure.
3. What position is best for enema administration?
The left lateral (Sims’) position is the best because it allows the enema solution to flow naturally into the colon, improving effectiveness and patient comfort.
4. How long should a patient retain an enema?
Patients are usually advised to retain the enema for 5–15 minutes, depending on the type of enema and patient tolerance.
5. What are the different types of enemas?
Common types include:
Cleansing enema
Oil retention enema
Medicated enema
Carminative enema
Each type serves a specific purpose in patient care.
6. Is enema administration painful?
Enema administration is generally not painful, but patients may experience mild discomfort or cramping. Proper technique and slow administration help reduce discomfort.
7. What complications can occur with enemas?
Possible complications include:Abdominal cramps
Rectal irritation
Fluid imbalance
Rarely, bowel perforation
Proper nursing care minimizes these risks.
8. When should an enema not be given?
Enemas should be avoided in patients with:Recent rectal surgery
Severe hemorrhoids
Rectal bleeding
Bowel obstruction
Always consult a doctor if unsure.
9. Can enemas be given at home?
Yes, enemas can be administered at home with proper guidance. However, it is important to follow instructions carefully and use safe, recommended solutions.
10. How much fluid is used in an enema?
The amount varies depending on the type of enema:
Adults: Typically 500–1000 mL for cleansing enemas
Children: Smaller volumes as prescribed
11. How can nurses ensure patient comfort during an enema?
Explain the procedure clearlyUse warm solutionAdminister slowlyMaintain privacy and dignity
12. What should nurses document after giving an enema?
Documentation should include:Type of enemaAmount of solution usedPatient responseResults (bowel movement)Any complications